Hello,
This week is the first in a 3-part series on ethics, which are part of both ABMGG and ABGC board exams.
Please feel free to email with any comments or questions about this post (daniel@studyrare.com).
Also, I’ve heard from a few graduating GCs that the job market is tough right now. If you are aware of any job openings for GCs at your institution, please feel free to send me any job posting(s) that you are aware of, and I will share them in the next newsletter.
Please share this post with anyone who might find it useful!
-Daniel
Questions
Question 50
A 32-year-old woman with a family history of breast cancer and a known pathogenic BRCA1 variant presents for follow up. She desires genetic testing for BRCA1 for her 3- year-old daughter, who is asymptomatic and developing normally. Which of the following ethical principles is most important to discuss with this patient regarding the testing of her daughter for the BRCA1 variant?
Question 51
A 22-year-old Spanish-speaking woman presents with a multi-year history of progressive neurological symptoms. The clinical team decides to pursue exome sequencing. While obtaining verbal informed consent through a language interpreter, the resident does not mention the option of secondary findings. After the visit, the medical student asks the resident why secondary findings were not discussed. The resident replies that “It would have been too complicated for her to understand the secondary findings, and we were running low on time.” The same resident had discussed the option for secondary findings with the previous two patients, where an interpreter was not required. This situation most clearly violates which sets of ethical principles?
Explanations
Q50: Autonomy
Q51: Autonomy and Justice
The four principles of medical ethics are beneficence (doing good), autonomy (the freedom to decide), nonmaleficence (do no harm), and justice (ensuring equity and fairness). Remember these as “BANJO!” These ethical principles are a common topic on board exams. They are also important to keep in mind when working with patients, as medical decision-making often requires tradeoffs between these principles.
Question 50
In this case of an asymptomatic minor (<18 years old), the principle of autonomy (Question 50) is most important to uphold. Autonomy refers to an individual's freedom to make decisions about their own healthcare. With few exceptions, genetic testing for adult-onset conditions (e.g., most hereditary cancer syndromes) is not recommended in children. In this case, the child is asymptomatic, and the knowledge of being a carrier would not impact their health until adulthood, when more intensive screenings would begin. Therefore, the patient (once they are an adult) should decide whether the benefits of genetic testing (e.g. opportunity for screening and early detection) outweigh the risks (e.g. insurance or workplace discrimination — see the exceptions to GINA). By allowing the child to make this decision for themselves as an adult, we respect their autonomy.
The principle of justice is less relevant in Question 50, as there is no shortage of resources mentioned in this question. There are also no concerns about the fair or equitable treatment of the child that would be related to justice. Beneficence is less important to consider in this questions, as there is no opportunity for genetic testing to improve her health at her current age. Nonmaleficence, or the obligation to do no harm, is also not at the center of this particular question. The child’s health would not be immediately harmed as a result of doing (or not doing) this test.
Question 51
In this scenario, the ethical principles of autonomy and justice were clearly violated. The resident did not respect the patient’s autonomy to decide for themselves whether they would like to know secondary findings that could potentially result in earlier screening and detection for cancer or heart disease. In addition, the resident did not treat the patient equitably based on their limited English proficiency, which violates the principle of justice.
The principle of justice
At its core, justice is about treating patients fairly and equitably. In this example, the resident perhaps grew impatient with the length of the visit and deciding to cut corners with the consent. Under an equitable approach to patient care, the resident would have gone through the entire consent with this patient, even if it meant a longer visit compared to his previous patients.
💡Remember that medical visits requiring an interpreter take twice as long to convey the same amount of information (because everything needs to be said twice!)
In addition, the resident’s assumption about the woman’s ability to comprehend health-related matters also likely contributed to his decision to skip part of the consent. This is an example of unfair treatment, as the same medical decision that was discussed with the previous patients was not discussed with her. It is well-established that unfair treatment in the U.S. healthcare system occurs more often among women, racial and ethnic minorities, people who identify as LGBTQ, and individuals with limited English proficiency. It is also important to note that low English proficiency does not imply low health literacy or low comprehension ability. In all cases, it is the duty of the healthcare provider to conduct the encounter in a manner that the patient can understand, and to discuss all available medical decisions in a non-judgmental manner.
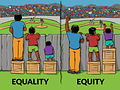
💡Equal treatment is not the same as equitable treatment. In fact, there are several aspects of our healthcare system that treat patients equally and inequitably at the same time. One example of this is the fact that medical clinics allocate an equal amount of time per patient visit, regardless of language. I challenge you to think about what healthcare inequities exist in your hospital or clinic, and how you can work to provide more equitable patient care (comment below!)
Examples of equitable treatment
There are multiple examples of equitable treatment of disadvantaged individuals in our society. Some examples include accessible parking spaces near the entrances to buildings for individuals with certain physical disabilities, accommodations on standardized tests for students with attention deficit disorder, and preferred housing for low-income individuals with HIV living in NYC.

Distributive justice
Distributive justice is another form of justice often discussed in healthcare settings. The concept of distributive justice reflects the equitable allocation (i.e. distribution) of healthcare services throughout society. One recent example was during the COVID pandemic, when healthcare providers had to ration ventilators and other medical equipment due to high demand. The development of protocols for deciding how to allocate these scarce resources among critically-ill patients was an example of distributive justice in action.
Learning objective
There are 4 main ethical principles (“BANJO”): beneficence, autonomy, nonmaleficence, and justice. Healthcare providers should adhere to these principles when participating in any medical decision-making process, including obtaining informed consent. The principle of justice involves treating patients both fairly and equitably, as well as considering how limited resources are distributed in society (distributive justice).
2023 ABMGG General Exam Blueprint | X. Genetic Counseling → c) Ethical issues → i) Autonomy, beneficence, non-maleficence, justice (page 5)
References
Principles of Clinical Ethics and Their Application to Practice (2020)